Breast Reconstruction in St. Louis
Our surgeons specialize in a variety of Plastic Surgery procedures of the chest including all forms of aesthetic and reconstructive breast surgery from breast augmentations, lifts, reductions, to breast cancer reconstruction. Here at St. Luke’s they help treat and reconstruct women throughout the spectrum of breast disease, from those that have been deemed to have a high-risk genetic mutation, to those who have been diagnosed with invasive breast cancer and decide to undergo mastectomy.
Breast reconstruction is without a doubt one of the areas our surgeons are most passionate about. Being diagnosed with breast cancer is an emotional roller coaster ride, and it is our job to help you see the light at the end of that tunnel. Women sometimes have to undergo a variety of imaging and biopsy procedures, and meet with many different doctors from the breast surgeon, to the medical and radiation oncologists, and also their reconstructive surgeon. Our surgeons and staff understand this is a very stressful time and will do everything possible to make you feel more comfortable. Our number one goal is to cure your cancer. Your surgeon will then help recreate a natural-appearing and feeling breast that makes you feel whole again. Often times they can start this reconstructive process immediately at the time of your cancer operation, using the same incision, and you can wake up already on your way to normalcy. This truly helps with the emotional and physical recovery process.
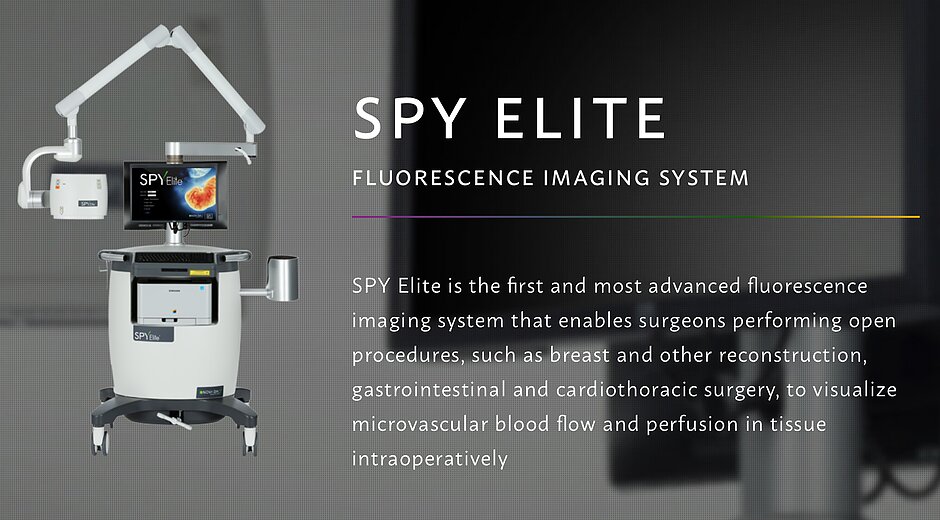
Here at St. Luke’s, our surgeons are part of a multi-disciplinary team of specialists who work closely together to provide state-of-the-art breast cancer care and reconstruction. They discuss your care plan as a team, ensuring you have the best possible outcomes. In the operating room, our surgeons often use one of the most sophisticated intraoperative imaging systems (SPY Elite) allowing them to visualize the microvascular blood flow and tissue perfusion in real-time. This ensures optimal outcomes for our most advanced reconstructions.
BREAST PROCEDURES
- Immediate and Delayed Breast Reconstruction
- Staged Tissue Expander Reconstruction
- Direct to Implant Reconstruction
- Subpectoral Reconstruction
- Prepectoral Reconstruction
- Pedicled Transverse Rectus Abdominus Muscle (TRAM) Flap Reconstruction
- Pedicled Latissius Flap Reconstruction
- Thoracodorsal Artery Perforator (TdAP) Flap Reconstruction
- Revision Breast Reconstruction
- Oncoplastic Reconstruction
- Fat Grafting
If undergoing mastectomy and reconstruction on only one breast, our surgeons will discuss symmetry procedures (if needed) to your remaining breast to ensure you look and feel your best. This may include:
Don’t worry, these procedures are also covered under insurance by law (Women’s Health and Cancer Rights Act). Learn more here:

INITIAL CONSULTATION
Your surgeon will review your cancer and medical histories, anticipated cancer treatment options, and prior surgeries. They will discuss your current breast size, body type, and your specific goals as well as your concerns. They will examine your abdomen, back, extremities, and breasts, as well as take some measurements to help guide your choices. Breast reconstruction is a beautiful blend of artistry and science, and this helps personalize your options including implants or methods using your own tissues. Your surgeon will show you examples of breast devices, from tissue expanders to a variety of the latest generation implants. You will get to touch and feel the devices, and your partner or family will too. They will go over diagrams of the procedures, and extensively discuss all of the risks & benefits. Our surgeons are strong proponents of “knowledge is power” and want you to feel empowered, comfortable, and confident in whatever reconstructive journey we agree to embark upon.

IMPLANT-BASED BREAST RECONSTRUCTION
Implant-based reconstruction is by far the most common method chosen by women in America today. It means a new breast mound will be built based on a saline or silicone gel-filled device. Sometimes this can happen in a single procedure (direct-to-implant reconstruction), immediately after the cancer operation. More often, however, this is a staged procedure where a “tissue expander”, or medical balloon, is first placed in the desired breast location. This expander is filled with sterile fluid at the time of surgery, and several times thereafter in the Chesterfield Plastic Surgery office. This is usually done on a weekly basis and most patients do not have much discomfort during this process. Once you reach your size goal, time is allowed for the tissues to relax and get accustomed to the newly stretched size and shape for 1-3 months. Your surgeon will then exchange this tissue expander for the softer, more natural permanent implant at a second, much less stressful surgery and usually you go home later that day.
Our surgeons are proficient in all forms of implant-based reconstruction. Based on your current and desired reconstructed breast size, coupled to your cancer location and treatment plan they will discuss a variety of techniques applicable to you. This includes pre-pectoral, partial submuscular, full submuscular, and breast reduction-reconstruction techniques. They are well versed in the latest implant and acellular dermal matrix technologies to achieve excellent results in the safest, most reliable manner possible.
Click HERE to watch an animation about our most common breast reconstruction technique using an acellular dermal matrix such as Alloderm to support the implant like a hammock. This allows our surgeons to precisely control the breast fold and outer breast border, all while keeping the breast skin happy. This animation is also similar to the “pre-pectoral” technique our surgeons frequently use. In these cases, the muscle is left alone and a larger piece of Alloderm is tented over the entire implant and secured to the chest wall, rather than the lower portion of the muscle.

AUTOLOGOUS TISSUE RECONSTRUCTION
Autologous tissue reconstruction is when your own tissues are used to build the breast. This is most commonly performed with the lower abdominal tissues, but can also be from the latissimus muscle on the back, or the tissues on one’s thighs or buttock. Here at St. Luke’s our surgeons perform the pedicled tissue transfer options meaning the blood supply remains attached to your body during the tissue transfer process. These are great options especially for reconstructing one side while the other breast remains larger and natural appearing. It is also a great option to incorporate at some point in time in your reconstruction if you have to undergo radiation as part of your cancer treatment. It has a longer recovery period, and as with any surgery has its own set of risks and benefits, all of which your surgeon will cover in your consultation.
Contact Us To Schedule A Consultation
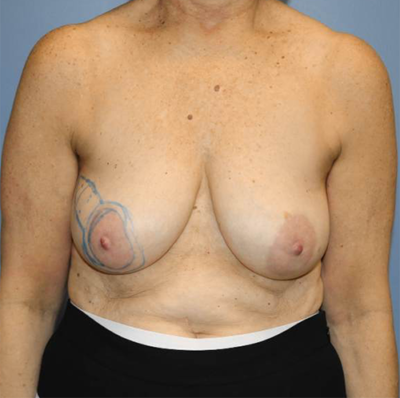
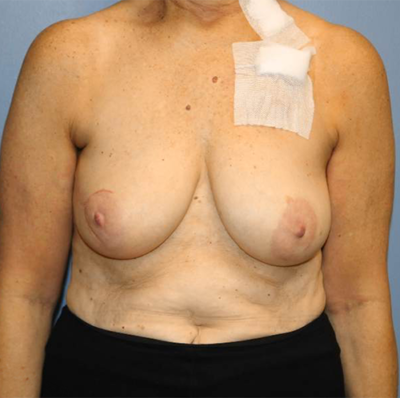
Breast Reconstruction Before & After
Click here to see more results
PREPARING FOR BREAST RECONSTRUCTION
Smoking and all forms of nicotine must be stopped at least 4 weeks prior to reconstruction. This includes e-cigarettes, patches, and gum.
Any medications and supplements which cause an increased risk of bleeding should also be stopped 2 weeks prior to any major surgery. Please see our list of medications and supplements to avoid. As always, make sure to check with your doctor before stopping any medications.
BREAST RECONSTRUCTION TECHINQUE:
On the day of surgery, your surgeon will draw the planned incision sites and any reference points necessary on areas to be operated on. Your breast surgeon and the operative team will bring you to the operating room, where the initial cancer operation to remove the tumor and sample any lymph nodes will be performed. Once this is complete, your surgeon will assess your tissues and begin your reconstruction. Some numbing medication will be injected during your surgery to help decrease postoperative discomfort. A small thin tube (surgical drain) will be placed to help remove fluid from the surgical sites as you heal. Several layers of dissolvable sutures will be used to meticulously close all operative sites, with a medical skin glue on top of this. Drain sites are covered with special antibacterial waterproof dressings so that you can shower the day you go home. You will be fit into a postoperative bra and transferred to the surgical floor where our specialized nurses will help you in your immediate recovery. Medications will be given to help ease any pain.

RECOVERY FROM BREAST RECONSTRUCTION
Most patients undergoing implant, expander, or oncoplastic reconstructions are allowed to go home the next day. Patients having autologous tissue or flap-based reconstructions typically need to remain in the hospital for 3-5 days for close monitoring. Your surgeon will usually remove some of your surgical drains at the first follow-up 1 week after surgery. Any remaining drains are usually removed at your 2-week office follow-up depending on the daily fluid output.
Postoperative soreness will be the greatest in the first 2-3 days as your body is beginning the recovery process. Many women then feel much better, with a significant relief once again after all of the drains are removed. Although you should plan to take 4-6 weeks off of work after your initial cancer operation and reconstruction, most women feel fair back to normal after about 3 weeks.
Most breast reconstruction patients will have some arm range of motion limitations for the first 3 weeks. This is necessary to allow your tissues to heal correctly without rubbing or shearing forces that can cause persistent fluid collections (seromas). Thus, your surgeon will usually request patients limit lifting of their arms past shoulder level or reaching far behind them. Any motion in front of the body is okay including eating, brushing teeth, washing your hair. Just don’t go reaching overhead for that item on the top shelf! It helps to wear button-up shirts for the first few weeks as well.

Breast Reconstruction FAQs
Do you Have a Question?
Return to ProceduresSee Our Specials